Learn More
Explore what our Behavioral Health Software can do for you.
Medicare Behavioral Health Integration (BHI)
Medicare's Behavioral Health Integration program is categorized under multiple CPT codes. Some of these codes are 99492, 99493, and 99494. These CPT codes are billed when BHI services are supplied using the Psychiatric Collaborative Care Model (CoCM) to patients during a calendar month.
According to Medicare, the CoCM model consists of four key components:
- The primary care team perform the initial assessment and are responsible for administering the validated rating scales.
- The primary care team’s joint care planning with the patient, with care plan revision for patient(s) whose condition isn’t improving adequately. Treatment may include pharmacotherapy, psychotherapy, or other recommended treatments.
- Behavioral health care manager following up proactively and systematically using validated rating scales and a registry.
- Regular case load review with psychiatric consultant at least weekly.
General BHI
CPT code 99484 is used to bill monthly services delivered using BHI models of care other than the psychiatric collaborative care model, or CoCM, that similarly include “core” service elements such as:
- Systematic assessment and monitoring
- Care plan revision for patients whose condition is not improving adequately
- Continuous relationship with a designated care team member
CPT code 99484 may be used to report models of care that do not involve a psychiatric consultant, nor a designated behavioral health care manager (although such personnel may furnish General Behavioral Health services). CMS expects to refine this code over time, as more information becomes available regarding other BHI care models in use.
Service Components:
- Initial assessment
- Initiating visit (if required, separately billed)
- Administration of applicable validated rating scale(s)
- Systematic assessment and monitoring, using applicable validated clinical rating scales
- Care planning by the primary care team jointly with the beneficiary, with care plan revision for patients whose condition is not improving
- Facilitation and coordination of behavioral health treatment
- Continuous relationship with a designated member of the care team
CARE TEAM MEMBERS
- Treating (Billing) Practitioner – A physician and/ or non-physician practitioner (PA, NP, CNS, CNM); typically primary care, but may be of another specialty (for example, cardiology, oncology, psychiatry).
- Beneficiary – The beneficiary is a member of the care team.
- Potential Clinical Staff – The service may be provided in full by the billing practitioner. The billing practitioner may also use qualified clinical staff to provide certain services using a team-based approach. The clinical staff may include staff or contractors who meet the qualifications for the CoCM behavioral health care manager or psychiatric consultant.
Eligible Conditions
Eligible conditions are classified as any mental, behavioral health, or psychiatric condition being treated by the billing practitioner, including substance use disorders, that, in the clinical judgment of the billing practitioner, warrants BHI services. The diagnosis or diagnoses could be either pre-existing or made by the billing practitioner and may be refined over time.
Synergy's Behavioral Health Software
Synergy's Care Management system provides Behavioral Health Software that is capable of tackling these kinds of tasks in a way that complies with Medicare's guidelines.
During patient care, our behavioral health software allows for multiple tasks on the same page in your native web browser. This helps you maintain your workflow while also being able to track all the necessary information during a BHI encounter.
In the BHI note, you are able to time the appointment while noting down the patient's symptoms or concerns. After your appointment is over, once you stop the timer, you can easily input the time into the left box. This will help your practice with billing and making sure you meet Medicare's requirements.
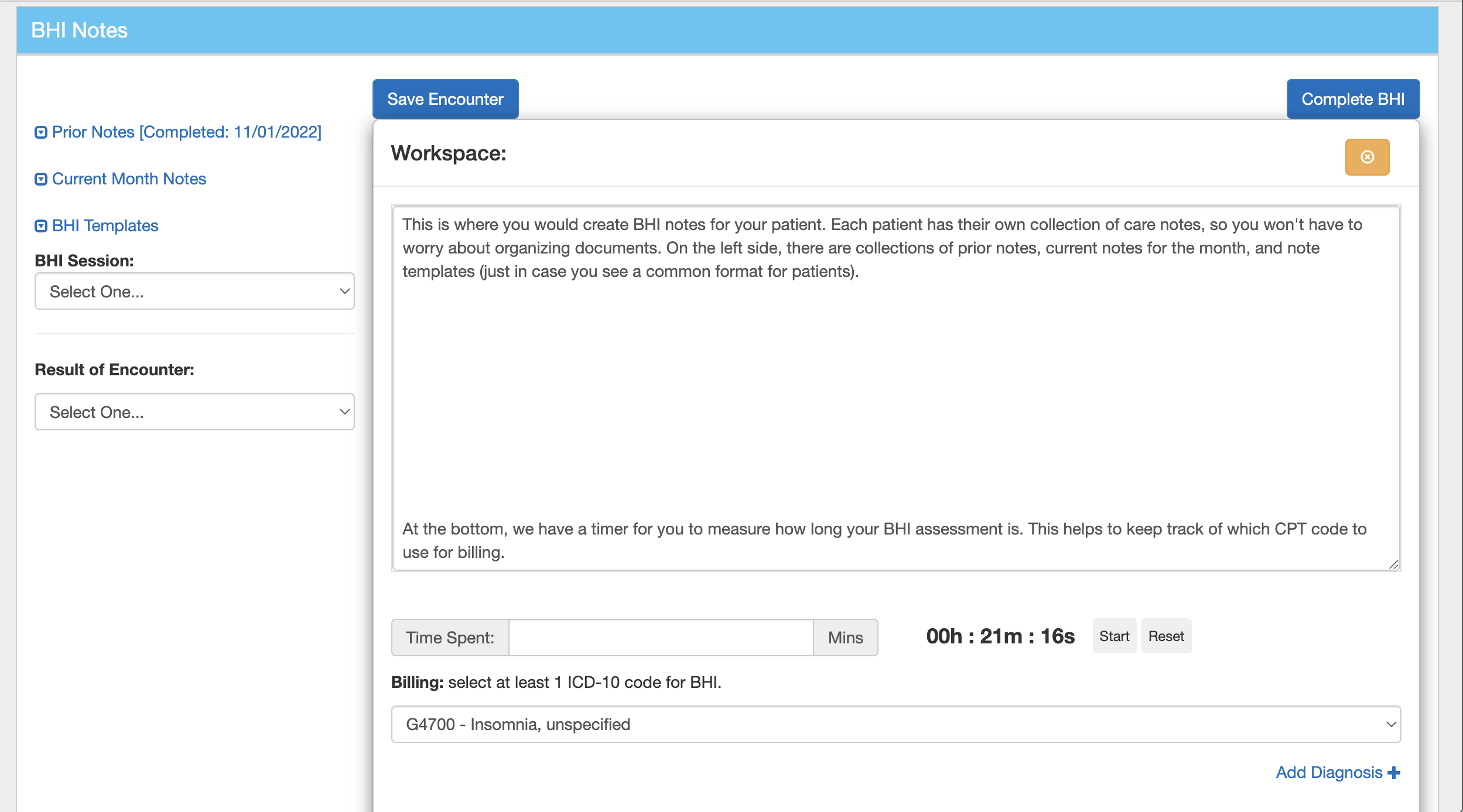
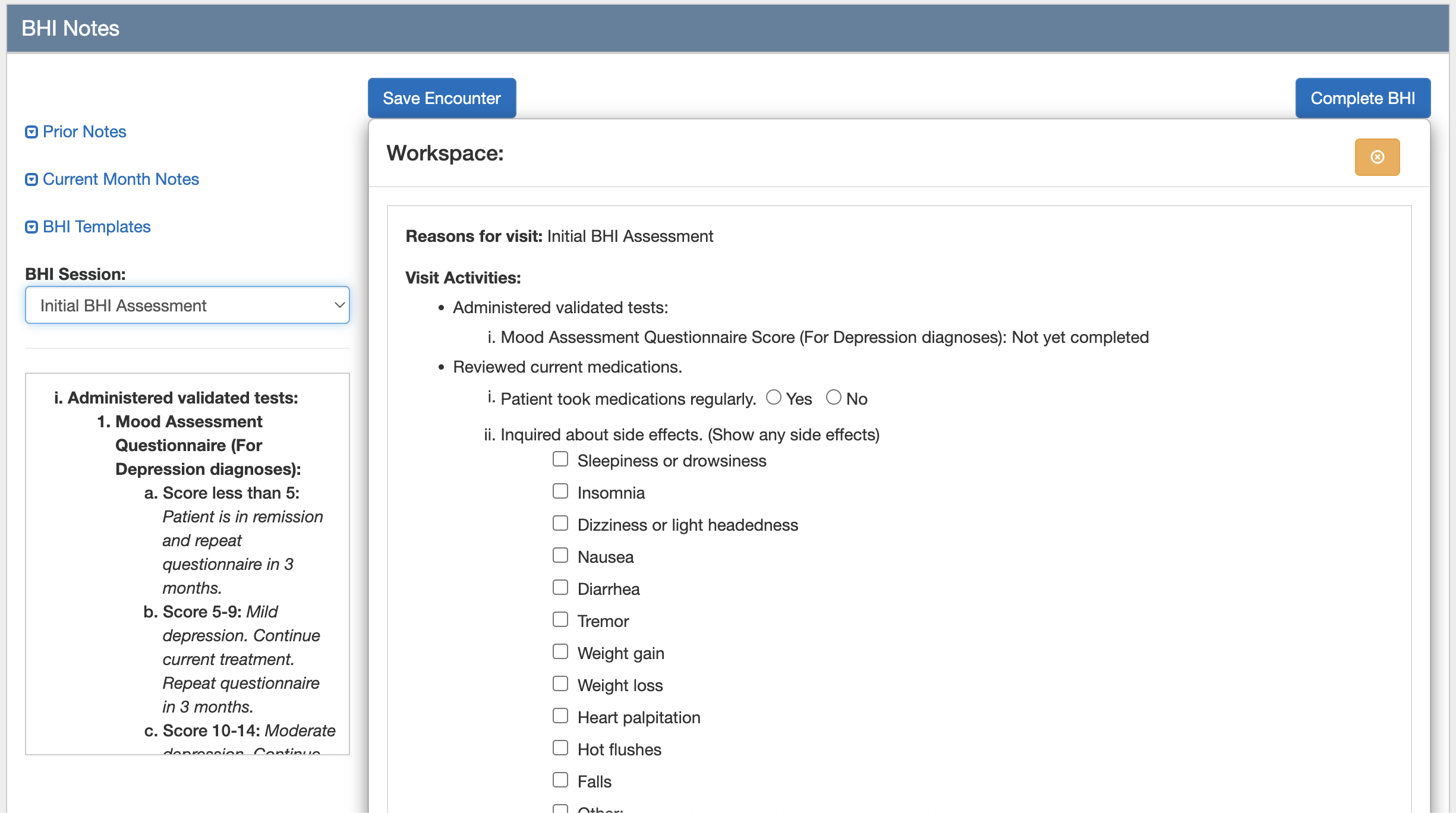
Our BHI templates list out all the tests and questionnaires you should go through with your patient to meet Medicare's requirements. We also calculate and compile each of the assessment scores and provide general care plans to help your patient.
Our software is built to streamline your workplace and create a more efficient care team.
